Actor portrayals.
Start your patients on the only non‑opioid, intrathecal option
Efficacy and dosing
INDICATION
PRIALT® (ziconotide) solution, intrathecal infusion is indicated for the management of severe chronic pain in adult patients for whom intrathecal (IT) therapy is warranted, and who are intolerant of or refractory to other treatment, such as systemic analgesics, adjunctive therapies, or IT morphine.
Clinical studies and safety
The efficacy of intrathecal PRIALT in the management of severe chronic pain was studied in three double-blind, placebo-controlled, multicenter studies in a total of 457 patients (268 PRIALT, 189 placebo). The first two studies utilized a fast titration schedule that resulted in less tolerability and substantially more frequent adverse events. Therefore, the third study utilized a slow titration schedule as follows1:
- Randomized, double-blind, placebo-controlled study of PRIALT using the 21‑day slow titration schedule
- Conducted in adult patients with severe chronic pain not adequately controlled with intrathecal analgesics, including morphine, bupivacaine, and/or clonidine; or who were intolerant to analgesics and/or systemic analgesics
- Dosing with PRIALT was started at 2.4 mcg/day (0.1 mcg/hr)
- Dosing was increased by 2.4 mcg/day (0.1 mcg/hr) two to three times/week (minimum titration interval 24 hours) to a maximum dose of 19.2 mcg/day (0.8 mcg/hr) as needed for management of pain
- Final mean dose at the end of the trial at 21 days was 6.9 mcg/day (0.29 mcg/hr)
Slow titration, low-dose study results
The mean baseline pain scores in both the PRIALT and placebo groups were 81 mm on the VASPI (0-100 mm scale). After 3 weeks of treatment, the mean percent change in VASPI score from baseline improved by a mean of 12% in the PRIALT group vs 5% in the placebo group (intent-to-treat analysis; 95% [0.04%, 13%]).1,2

For adverse reactions in the slow titration, placebo-controlled trial, by percent, that occurred in ≥5% of patients and more commonly with PRIALT than with placebo, see Table 1 in Section 6.1 of the Prescribing Information.
The most frequently reported adverse reactions (≥25%) in clinical trials were dizziness, nausea, confusional state, and nystagmus.1
*As per mean percent change in Visual Analog Score of Pain Intensity (VASPI) score from baseline to Day 21 for both groups.1,2
PRIZM registry3
The Patient Registry of Intrathecal Ziconotide Management (PRIZM) was a real-world, prospective, multicenter, observational 18-month registry of 93 ziconotide patients with severe chronic pain.
- Objectives: Evaluate the short- and long-term safety and effectiveness of IT ziconotide based on patient-reported outcomes
- Primary efficacy outcome: Change in numeric pain rating scale (NPRS) score from baseline to Week 12 after enrollment
- NPRS scores were assessed at every clinic visit, including at 6, 9, 12, 15, and 18 months
Observational analyses are NOT intended for direct comparison with clinical trials and may introduce bias. Real-world evidence can complement data from randomized controlled trials. The data presented below is observational and come from ad hoc, non-prespecified analyses. No conclusions of statistical or clinical significance can be drawn.
The results of patients who were given PRIALT as monotherapy are presented below:
- 93 patients enrolled in the study, 74 patients completed 12 weeks (primary endpoint), and 60, 46, 37, 30, and 28 patients remained in the registry at 6, 9, 12, 15, and 18 months
- 86% of patients were on ziconotide monotherapy at Week 12, 74% at Month 6, 55% at Month 12, and 57% at Month 18
- Mean reduction in pain intensity level (NPRS score) over baseline was greater in the monotherapy group and led to a greater percentage of patients with a clinically meaningful response (30% reduction in NPRS score) at all time points
- Week 12: 26%; Month 6: 41%; Month 9: 44%; Month 12: 50%; Month 15: 60%; Month 18: 43%
Almost all patients experienced adverse events, the most common of which were nausea (25.8%), confusional state (22.6%), and dizziness (20.4%). The treatment-emergent adverse event profile was similar to what was observed in the clinical trial program.1
NPRS=numeric pain rating scale.
When to prescribe PRIALT – the only FDA-approved, non-opioid, intrathecal treatment for severe chronic pain
According to the 2016 Polyanalgesic Consensus Conference (PACC) guidelines, intrathecal therapy occupies the same line of management as neurostimulation, with important caveats regarding your patient's condition4:
- Before in patients with active cancer-related pain that is mechanical and likely to spread (level III, grade C)†
- Within the same line in patients with non-cancer pain (level III, grade C)†
- After for non-cancer pain if the pain is isolated and unlikely to spread (level III, grade I)†
†Recommendation made using United States Preventive Services Task Force (USPSTF) criteria. Evidence level III: Clinical experience-based opinions, descriptive studies, clinical observations, or reports of expert committees; Recommendation grade C: Neither recommendable nor inadvisable (at least moderate evidence that the measure is effective, but benefits are similar to harms and a general recommendation cannot be justified); Recommendation grade I: Insufficient, low quality, or contradictory evidence; the balance between benefit and harms cannot be determined.4
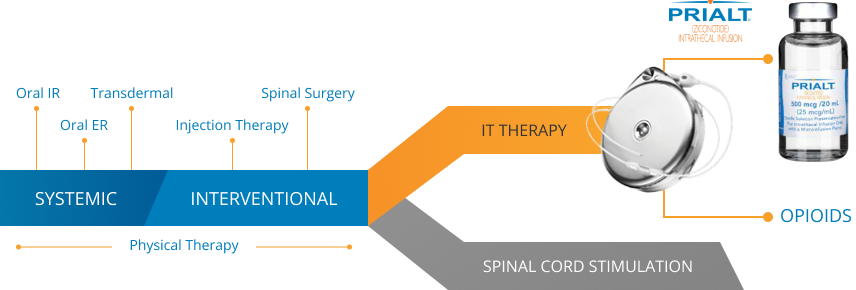

ER=extended release; IR=immediate release.
First-line recommendation4
Evidence supports PRIALT efficacy in localized and diffuse non-cancer pain.4
Ziconotide, the analgesic agent of PRIALT, was identified as one of two preferred first-line IT options and included in the highest level of recommendation (level I, grade A)‡ for those with non-cancer pain.4
‡Recommendation made using USPSTF criteria. Evidence level I: At least one controlled and randomized clinical trial, properly designed; Recommendation grade A: Extremely recommendable (good evidence that the measure is effective and benefits outweigh the harms).4
Steps for starting your patients on PRIALT
Establish patient expectations of intrathecal therapy:
- Explain that PRIALT is FDA-approved and PACC guideline-recommended for adults with severe chronic pain1,4
- Discuss the goals of treatment and that it may take time to respond1
- Educate patients on potential adverse reactions and monitor their response to treatment1
- Recommend psychological evaluation of patients to monitor for issues4
- Continually monitor patients' progress and assess their response to treatment, including improvements to pain severity1
Start slow
According to the 2024 PACC Guidelines, the recommended starting dose for continuous IT delivery of PRIALT is 0.5-1.0 mcg/day—within the limit of no more than 2.4 mcg/day stated in the Full Prescribing Information.1,5
Consensus Point 23 – When titrating IT ziconotide dosing, an increase of ≤0.5 mcg/day with weekly reassessment is warranted (level I, grade B, certainty moderate).5§
§Recommendation made using USPSTF criteria. Evidence level I: At least one controlled and randomized clinical trial, properly designed4; Recommendation grade B: The PACC recommends the service or concept. There is high certainty that the net benefit is moderate, or there is moderate certainty that the net benefit is moderate to substantial. A moderate level of certainty means the available evidence is sufficient to determine the effects of the preventive service on health outcomes, but confidence in the estimate is constrained by various factors.5
Titrate to effect
Dosing example based on 2024 PACC Guidelines:


Assess each patient's response to therapy regularly to determine if a dose increase or decrease is required. Not all patients will require the same dose.
Monitor adverse events to manage outcomes
2024 PACC Guidelines also recommend:
Consensus Point 24 – When side effects occur, it is recommended to reduce the IT infusion dose of ziconotide to the last tolerated level that relieved pain without side effects. In the setting of severe side effects, it also is recommended that ziconotide can be discontinued without the risk of withdrawal (level II, grade B, certainty moderate).5¶
¶Recommendation made using USPSTF criteria. Evidence level II: Expert opinion based on risk-benefit or on case reports; Recommendation grade B: The PACC recommends the service or concept. There is high certainty that the net benefit is moderate, or there is moderate certainty that the net benefit is moderate to substantial. A moderate level of certainty means the available evidence is sufficient to determine the effects of the preventive service on health outcomes, but confidence in the estimate is constrained by various factors.5
References: 1. PRIALT® (ziconotide). Prescribing Information. TerSera Therapeutics LLC. 2. Rauck RL, Wallace MS, Leong MS, et al. A randomized, double-blind, placebo-controlled study of intrathecal ziconotide in adults with severe chronic pain. J Pain Symptom Manage. 2006;31(5):393-406. 3. McDowell GC, Saulino MF, Wallace M, et al. Effectiveness and safety of intrathecal ziconotide: final results of the Patient Registry of Intrathecal Ziconotide Management (PRIZM). Pain Med. 2020;21(11):2925‑2938. 4. Deer TR, Pope JE, Hayek SM, et al. The Polyanalgesic Consensus Conference (PACC): recommendations on intrathecal drug infusion systems best practices and guidelines. Neuromodulation. 2017;20(2):96-132. 5. Deer TR, Hayek SM, Grider JS, et al. The Polyanalgesic Consensus Conference (PACC)®: intrathecal drug delivery guidance on safety and therapy optimization when treating chronic noncancer pain. Neuromodulation. 2024;27(7):1107-1139.
SUPPORT FOR YOU AND YOUR PATIENTS
Learn about PRIALT coverage support and download resources